Next Steps
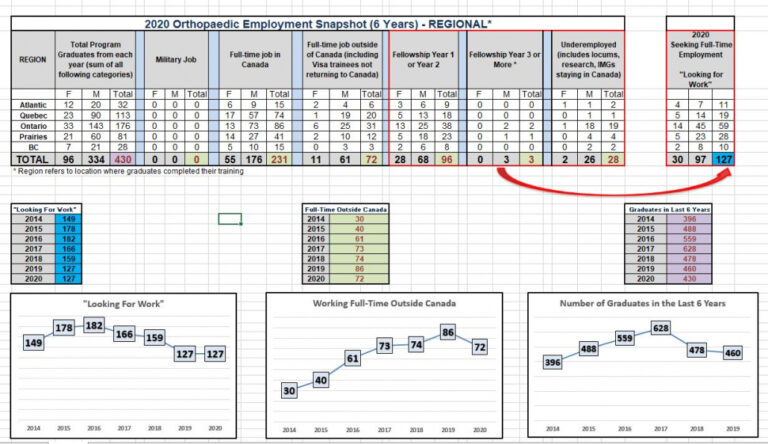
Persistent underfunding of MSK care has led to ongoing underemployment among orthopedic surgeons in Canada. Despite slight improvements, there are still more surgeons entering the job market than there are positions available. The reduction in training positions and the rising trend of graduates moving to the U.S. for work further exacerbate the issue.
In a report, the Royal College of Physicians and Surgeons of Canada released findings from their annual Royal College Employment Study (Royal College Employment Study, 2019) based on a survey of medical specialists newly certified in 2017 about their job prospects.
The top six barriers to employment are:
-
- Too few available positions in Canada
- Poor access to job listings
- Desire or need to stay near family
- The need for spousal employment
- Lack of available health care resources (e.g. funding, operating room time)
- The delayed retirement of established physicians and surgeons (and their general reluctance to share resources)